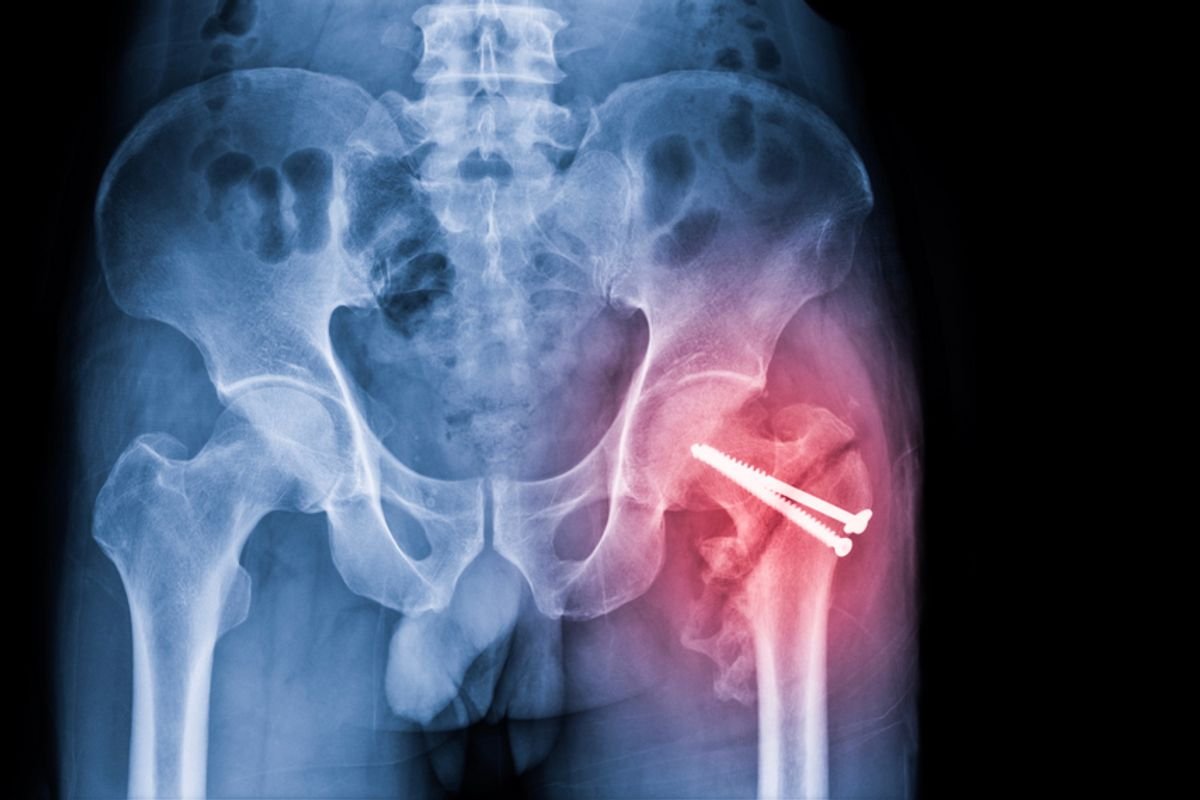
Hip Fractures Can Signal More Than a Broken Bone in the Elderly — Sometimes with Fatal Consequences

Just as we might not recover from falling out of a swing in our twenties or thirties as quickly as we might’ve bounced back as children, the amount of time and effort it takes to recover from an injury increases as we age. This is especially the case with hip fractures, which are a common yet severe injury that an older adult can sustain in their lifetime.
As human lifespans increase and populations age, the number of hip fractures older adults sustain is also projected to increase. In a 2020 study in Clinical Orthopaedics and Trauma, approximately 1.6 million hip fractures were estimated to occur worldwide each year, with the number projected to increase to 2.6 million by 2025 and 4.5 million by 2050.
Hip fractures, though they may sound innocuous, are not as simple as a broken bone. Elderly patients can face a plethora of health issues following surgical treatments, with even death as a potential risk following the injury itself or post-operative complications.
“Even though, for the most part, the general public is aware that this can be a sentinel, poor-prognostic event in older people, it’s remarkable how many people don’t quite appreciate that,” Howard Chansky, chair of the Department of Orthopaedic Surgery and Sports Medicine at the University of Washington Medicine, told Discover. “They might feel like, ‘Okay, this is a broken bone. You fix it.’ But it’s important that families and patients understand this is a serious event for an older person, and it’s helpful to start preparing them for how difficult the recovery is.”
Read More: What People Who Lived Past 110 in Brazil Reveal About Health Span — Not Lifespan
What Causes Hip Fractures
Several factors can lead to a hip fracture, though osteoporosis is a common cause, particularly in older women. Balance issues, cardiovascular issues, diabetes, anemia, and other underlying diseases, as well as the loss of muscle mass that comes with aging, are other examples of factors that predispose elderly people to hip fractures.
But while accidental falls are a common reason someone might fracture their hip, even something as simple as getting up or walking could result in an injury. Those types of fractures, Chansky added, are pathological, meaning they occur in bone that is abnormal and structurally weak — a bone weakened by osteoporosis or cancer, for example, takes much less energy to break than a bone without either.
These underlying factors are why fracturing a hip is comparatively more dangerous than breaking an arm or leg, for example.
“What specifically makes hip fractures so dangerous in the elderly is the fact that it’s typically a sign of something else going on,” Anthony Wiggins, assistant professor in the Division of Arthritis and Joint Replacement at the University of California, San Francisco’s Department of Orthopaedic Surgery, told Discover. “Whether that is someone with osteoporosis or someone that’s malnourished, it’s basically a sign that something’s underlying.”
Why Hip Fractures Might Cause Death
According to a 2025 study in Medical Sciences, experts are increasingly calling for a reframing in the way doctors view and treat hip fractures — less so as a single consequence of trauma, but rather as an event involving multiple systems, from declining musculoskeletal systems to weakening immune systems to even metabolic disruption. Researchers in a 2023 study in The Journal of Personalized Medicine have also found that specific conditions prior to the injury, such as malnutrition and the use of anticoagulant medications, were also associated with higher mortality rates.
“Our immune systems don’t function as well when we’re older. Respiratory and cardiovascular function isn’t the same when we’re older, either,” Chansky said. “When you’re immobilized after a lower extremity fracture like that, it just increases the odds of the complications that go along with fractures in anybody.”
Those complications include further loss of muscle mass, pneumonia, bed sores, urinary tract infections, and blood clots. Patients may be at higher risk of heart attacks and even delirium following operations as well.
Ultimately, these fractures set off a cascade of health events in older people, including increased risk of further fractures and other injuries.
How to Recover From a Hip Fracture
In older adults, immobility and bed rest can be especially dangerous because many of these complications can stem from this. Operating on the injury within 24 to 36 hours of the initial injury is important, though getting them up and moving after surgery is just as crucial.
“What you don’t want is for people to be stuck in bed. For older people with higher risks or chances of developing complications, staying in bed is the last thing you want,” Wiggins told Discover. “You have to get to these injuries quickly, and you have to get to them in a way that allows them to get up and move.”
Moving around can start small — as long as movement is happening, and as soon as possible.
“Being in a chair is better than being in bed. Being up and walking, even in a walker, is better than being in a chair,” Chansky told Discover.
Recovering from a hip fracture, Chansky added, is not just a surgical problem. Multidisciplinary care involving a team of orthopaedic surgeons, geriatricians, physical therapists, and hospitalists, for example, is key for improved outcomes.
How to Prevent Hip Fractures
On a national scale, hip fractures are highly expensive injuries, racking up billions in healthcare expenditures every year. But some measures can reduce the likelihood of their occurrence in elderly patients.
Prevention can start with effective screening and ongoing long-term care with your primary providers. Those who are at higher risk for osteoporosis, especially older women, should have their bone health evaluated and consider medications that can increase their bone mass and strength, lowering their risk of pathological fractures, Chansky said. Staying up to date with the state of their bone health following a fracture is also important for geriatric patients.
“Resistance training is key,” Wiggins added. “Weightlifting or some sort of resistance training to continue to load the bones, because loading the bones is what leads to stronger bones.”
Avoiding potential fall risks, such as loose rugs or pets running around, and installing rails and nightlights around the house may also lower the risk of hip fractures. Keeping up with proper nutrition and supplementation (including vitamin D and calcium), considering alternatives to medications that can affect alertness and balance, and even wearing cushioned hip pads in patients at higher risk of falling are all ways to prevent a hip fracture.
But these same tactics — from optimized nutrition to movement to evaluating and treating their bone health — aren’t just isolated to preventative measures.
“A lot of the things we talk about for prevention are the same things to help optimize the recovery process,” Wiggins said. “They’re going to want to do all these things as soon as they’re able to: try to do some sort of resistance training, work with physical therapy, optimize their diet, take medicine if they need to, to improve bone density.”
This article is not offering medical advice and should be used for informational purposes only.
Read More: Aging Brains Show Surprising Mix of Decline and Adaptation
Article Sources
Our writers at Discovermagazine.com use peer-reviewed studies and high-quality sources for our articles, and our editors review for scientific accuracy and editorial standards. Review the sources used below for this article: